Calendar
April 2024 M T W T F S S « Jun 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 -
Recent Posts
Recent Comments
Archives
Categories
Author Archives: owner
Gum Disease
 Gum disease, also known as periodontal disease is a chronic intra-oral bacterial infection that does have systemic health implications.
Gum disease, also known as periodontal disease is a chronic intra-oral bacterial infection that does have systemic health implications.
We know that periodontal disease has significant infectious and inflammatory components and that it increases insulin resistance. Chronic inflammation and insulin resistance are both primary causes of athlerosclerosis, and athlerosclerosis is the primary driver of heart attacks and strokes.
Posted in Gum Disease, Periodontal Disease
Leave a comment
Fluoridated Water
What is fluoride, and why do we need it?
Fluoride is a naturally occurring mineral. Decades ago, health official’s realized that areas with high levels of fluoride in their water also had less tooth decay, spurring efforts to add fluoride in areas with lower levels. When you eat sugar or other refined carbohydrates, bacteria in the mouth produces acid that removes minerals from the surface of the tooth. Fluoride helps remineralize the tooth surface and prevent cavities,according to the federal Centers for Disease Control and Prevention.
Is the water supply the best way to deliver fluoride?
Health officials think so, because people take in water throughout the day, getting cavity protection. It also helps protect people who cannot afford regular dental care, a growing population in the current economic climate. “You don’t have to remember to do anything,” Bailey says. “It reaches people of all socioeconomic groups.”
What do I do if I don’t have fluoridated water?
Dr. Craig Oldham, president elect of the Hillsborough County Dental Association, recommends fluoride supplements for children 12 and under who live in areas without fluoridated water. “daily brushing is not enough,” he said, pointing out that ingesting fluoride not just placing it on the teeth is essential for tooth formation in children. Also, research has found that as people age and saliva production declines, fluoridated water also is protective.
Source: St. Petersburg Times, Thursday October 6,2011
By: RichardMartin
Posted in Periodontal Disease
Leave a comment
Transition baby from a bottle to a cup
By: Susan Sorensen
pediatrician
By the time most babies are about 9 months old, they have the motor skills to drink from a cup, so I recommend starting then. At first, fill a sippy cup with water and let your child experiment with it. Expect him to dribble and spit — that’s part of the fun. Within a few weeks, he’ll get the hang of it and before you know it, he’ll be willing to take all of his drinks from the cup.
Work toward a complete transition to the cup by about 13 to 14 months. The longer babies hang onto their bottles, the more attached they get to them. Switch to a cup before your baby is too attached, and you’ll save yourself a lot of frustration. If the bottle is your baby’s security object and he’s reluctant to part with it, let him choose a special sippy cup, maybe one that has pictures of a favorite character or animal on it.
What’s so horrible about toddlers drinking from bottles? If you’ve ever seen a picture of a child with bottle tooth decay, a.k.a. “bottle rot,” you’ll toss out every single one of your baby’s bottles faster than you can say root canal!
A child’s teeth are susceptible to decay if he habitually nurses a drink with sugar in it — formula, milk, or juice. Every time he takes a drink, natural bacteria in his mouth feed on these sugars and attack the teeth for 20 minutes. If he’s taking sips from a bottle every few minutes for an hour, his teeth are exposed to the sugars for at least 80 minutes. Over time, that causes tooth decay. Children are less likely to nurse drinks for long periods of time if they’re offered in sippy cups.
The best way to avoid bottle rot is to give your child his drink and have him finish it within about 20 minutes. Then use a toothbrush or washcloth to wipe his teeth clean. Never put a baby in his crib with a bottle or sippy cup. If he falls asleep, tooth-decay causing sugars can pool in his mouth for hours.
http://your-kids-teeth.com/tag/bacteria/
Posted in Uncategorized
Leave a comment
A healthy mouth can save your life!
Posted on June 26, 2011 by Dr. Paul Caputo DDS
Untreated Dental Disease Sooner or later, the vast majority of adults suffer from either tooth decay or gum disease. One of the bacterial types implicated in gum disease is “Porphyromonas gingivalis” which works its way below the gum line. If allowed to flourish these nasty microbes attack gum and bone tissue. Once this tissue erodes, teeth slowly loosen, become infected and ultimately may need to be extracted. These same bacteria are now known to be implicated in heart disease, diabetes, stroke and pregnancy complications.
Non-surgical treatment options for gum disease including prices and cost can be found here.
Posted in Gum Disease, Periodontal Disease
Leave a comment
Periodontal Disease Stages
It is estimated that more than half of all adults age 35 and older have early to advanced stages of periodontal disease. Periodontal disease (PD) is the primary cause of lost teeth after the age of 35 – not dental cavities!

What is periodontal disease ?
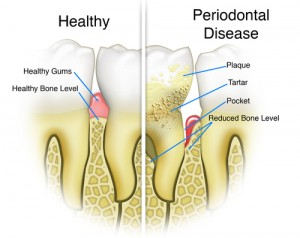
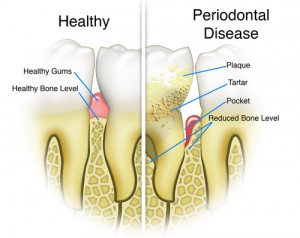
Periodontal disease is a chronic gum infection caused by plaque resulting in loss of bone support around the roots of teeth. Plaque is a thin film of bacteria that forms on teeth. Plaque converts to tartar if not cleared form teeth after 24hrs. Tartar irritates gums leaving them red, swollen and bleeding readily.
Eventually the gums peel away form teeth and create small pockets between the teeth and gums, slowly continuing to also destroy the supporting bone. Severe loss of the supporting bone is what loosens up teeth and make them incapable of functioning properly. Periodontal disease is often painless and will go undetected until bone loss is so severe that teeth are so loose they need to be extracted.
What are the signs ?
Early Stages:
• Bleeding gums when you brush or floss
• Red, swollen, tender gums
• Gums that have receded or shrunken away from teeth
Later Stages:
• Loose teeth, or teeth that have moved, or more spacing between teeth (especially front teeth) resulting in changes in bite or in the fit of dentures
• Foul smell or taste and/or pus that can be expelled when pressing on the gums
What can you do ?
The best way to treat periodontal disease is by early detection and prevention. A thorough examination can tell if you are at risk. Once diagnosed with periodontal disease, one must try to prevent further loss of supporting bone and/or other teeth.
Treatment usually involves a thorough scaling and root planing to remove plaque and built up tartar, thus allowing healthy gums tissues to reattach to root surfaces of teeth. Clean surfaces of teeth must be maintained by meticulous home oral hygiene and routine check-ups and cleaning.
Remember: There is really no cure for this “silent tooth killer”; cleanings can only dramatically slow down the disease process. Only early detection and prevention can make the difference between premature loss of teeth and a full compliment of healthy strong teeth.
Source: http://www.drchoo.com/images/preventive04.gif
Posted in Gum Disease, Periodontal Disease
Leave a comment
Waterpik vs Floss
Pros & Cons: Floss
Dental floss is an inexpensive way to help keep your teeth and gums healthy. MayoClinic.com indicates that floss is effective for cleaning tight spaces between teeth and will also scrape up and down the sides of each tooth. This is important because if plaque is not removed it can become tarter, a risk factor for the early stage of gum disease called gingivitis, according to the ADA.
On the other hand, the mechanical nature of floss can be abrasive. “Flossing can be irritating for people who have sensitive gums and may actually cause bleeding in some people,” Hayes notes. Also floss can’t be used by people who wear braces because it won’t penetrate the wires in order to reach the gums, Hayes adds.
Pros And Cons: Waterpik
One benefit of a Waterpik is that it’s gentle on the gums and is less likely to cause bleeding in people with sensitive gums, according to Hayes. A Waterpic is also ideal for people who wear braces — water will get behind the metal wires and flush out food particles. A Waterpik is sometimes recommended for people who have active gum disease because it flushes out bacteria from deep pockets that form when gums pull away from the teeth. “Floss can’t reach these pockets,” Hayes says. The downside: A Waterpik doesn’t remove plaque from teeth as well as floss. “Flossing scrapes off the sticky film of bacteria, while a Waterpic just rinses it,” Hayes explains. MayoClinic.com says using a Waterpik isn’t a substitute for flossing.
Source: http://www.livestrong.com/article/287399-waterpik-vs-floss/
Posted in Gum Disease, Periodontal Disease
Leave a comment
Animals have problems with their teeth too!
Not only do humans get periodontal disease but animals can too. I found out that most wild animals avoid major dental problems simply just by dying before their teeth go bad. Wild animals tend to only live a few years unlike our pets. Wild and pet animals rarely get cavities because there diet doesn’t have sugary foods unless they eat people food.
The problem is that tartar sticks to the teeth and irritates the gums. Its better if you give your pet hard food and/or treats that help clean the teeth and gums. You also can see your vet on a regular bases and your pet might need there teeth cleaned every few years, it all depends on your pet mouth.
About age six for cats and dogs gum disease will start to dissolve the bone around their teeth, teeth drop out, and some times abscesses form. Unless there properly cared for. When gum disease is present your pets breath will have a smelly odor, brown deposits on the back of their teeth. There may also have a redness along the gumline.
When it gets to this point it’s uncomfortable for your pet to chew anything hard,so their is less chewing and the mouth gets worse that much faster. In some cases it gets so bad that it becomes untreatable by the vet and they will start to fall out or can be extracted by the vet.
I know it might sound strange to take your pet to the vet for cleans and extractions. Take look inside your pets mouth and see if they have any redness or swelling. Thank you for reading.

You make the choice for your pet!
Sources:http://www.usatoday.com/tech/columnist/aprilholladay/2005-03-04-wonderquest_x.htm
http://www.placervillevet.com/periodontal%20disease.htm
https://www.healthymouth.com/index.php?page=periodontaldisease&atype=dogs
Posted in Gum Disease, Periodontal Disease
Leave a comment
Periodontal Abscess
I enjoy researching videos, photos, and articles of periodontal disease. Its very interesting to me, Even more interesting is the fact that periodontal disease can be revered if taken care of early enough and properly by both a hygienist and yourself.
A periodontal abscess is rapidly growing bacteria located in a space between your teeth and gums called a periodontal pocket. The pocket deepens to the point that plaque, tartar, and/or food then becomes trapped within. The body’s immune system at this point cannot adequately combat the infection.
Periodontal disease is extreamly destructive; if you don’t have it properly treated it can result in irreversible damage to the surrounding ligaments and bone. This will ultimatley cause you yo lose the tooth/teeth.
When the plaque and calculus is removed by scaling and root planning; this creates a healthier environment, thereby eliminating the infection.
Enjoy this video, hope it helps you understand the process of periodontal disease and realize how important it is to maintain your hygiene visits and take proper at home care of your teeth.
Sources: http://www.myperio.com/abscess.html
Posted in Gum Disease, Periodontal Disease, Uncategorized
Leave a comment
Periodontal Disease
Gingivitis
*It seems as though the 300 or so types of bacteria that homestead in our mouths have a  biting sense of humor. We fight them tooth and nail to prevent cavities. Then, just as we think we’re flossing enough and brushing enough to stop cavities, bacteria burrow into another area-our gums. As we get older, neglect of our gums begins to catch up with us until, when we’ve reached age 35 or so, our dentist mentions gum disease.
biting sense of humor. We fight them tooth and nail to prevent cavities. Then, just as we think we’re flossing enough and brushing enough to stop cavities, bacteria burrow into another area-our gums. As we get older, neglect of our gums begins to catch up with us until, when we’ve reached age 35 or so, our dentist mentions gum disease.
The earliest and most treatable form of gum disease is gingivitis, a buildup of bacterial plaque that causes gums to redden, swell and bleed easily. Although this kind of gum disease is painless, failing to treat gingivitis can lead to periodontitis, a condition that eventually causes tooth loss.
Brushing after meals and daily flossing comprise the one-two punch that can help keep your gums in the pink. But beyond the basics, here are some other ways to help put the bite on gingivitis.
What happens if you ignore the sore, bleeding gums that are a sign of gingivitis? You risk more serious periodontal disease and the possible loss of teeth.
Here are the signs that warn you your gingivitis is getting more serious. If you have any of them, see your dentist immediately.
• You have bad breath that doesn’t go away within 24 hours.
• Your teeth look longer-a result of your gums shrinking away from your teeth.
• Your mouth feels out of alignment when you shut it because your teeth come together differently.
• Your partial denture fits differently.
• Pus pockets from between your teeth and gums.
• Your teeth are loose, fall out or break off near the gum line.
Also, if your gums still bleed when you brush your teeth and continue to be sore and swollen despite your efforts at good oral hygiene, you need to see your dentist again.
Go electric.”Various studies show that you’ll remove more plaque with an electric toothbrush than brushing manually,” says Palm Harbor, Florida, dentist Paul Caputo D.D.S. The Interplak electric toothbrush removes 80 percent more plaque than a regular toothbrush, he says.
Add muscle to your mouth. Just as bones in the rest of your body can get brittle and shrink, so can your teeth and jawbone-making you more susceptible to gingivitis and other problems. “Calcium seems to help people with gingivitis, “says Dr. Caputo. “It strengthens bones and teeth.” Drinking two glasses of skim milk a day provides about 90 percent of your Recommended Dietary Allowance of calcium.*
The Doctors Book of Home Remedies II
By: Sid Kirchheimer and the editors of PREVENTION Magazine Health Books
1993
Posted in Uncategorized
Leave a comment